How closely linked are sleep apnea and hypertension? To what extent does obstructive sleep apnea contribute to the development of high blood pressure? When persons with sleep apnea utilize continuous positive airway pressure (CPAP), does their blood quality improve? Keep reading to get the details on all of this and more.
The link between obstructive sleep apnea and hypertension
Hypertension is the medical word for high blood pressure. If your systolic and/or diastolic blood pressure readings have been persistently high across many measurements, you have high blood pressure. Sleep apnea and pulmonary hypertension are related, however pulmonary hypertension is a distinct medical condition and deserves its own page. An average blood pressure reading should be about 120 over 80. In order to determine if you have prehypertension or hypertension, refer to the following blood pressure chart:
The most prevalent form of sleep apnea, obstructive sleep apnea (OSA), and the one most linked to cardiovascular problems including hypertension and heart disease, will be discussed in this article. A sleep apnea test is necessary for the diagnosis of obstructive sleep apnea (OSA), a sleep condition caused by disordered breathing during sleep characterized by repeated episodes of partial or complete throat closure. Chronic, excessively noisy snoring is a hallmark symptom of obstructive sleep apnea. Both in-lab and at-home sleep apnea tests (simply called sleep studies) are acceptable for this purpose. Sleep apnea is diagnosed when a doctor examines the results of a sleep study. Learn more for adapting to CPAP therapy for your sleep apnea.
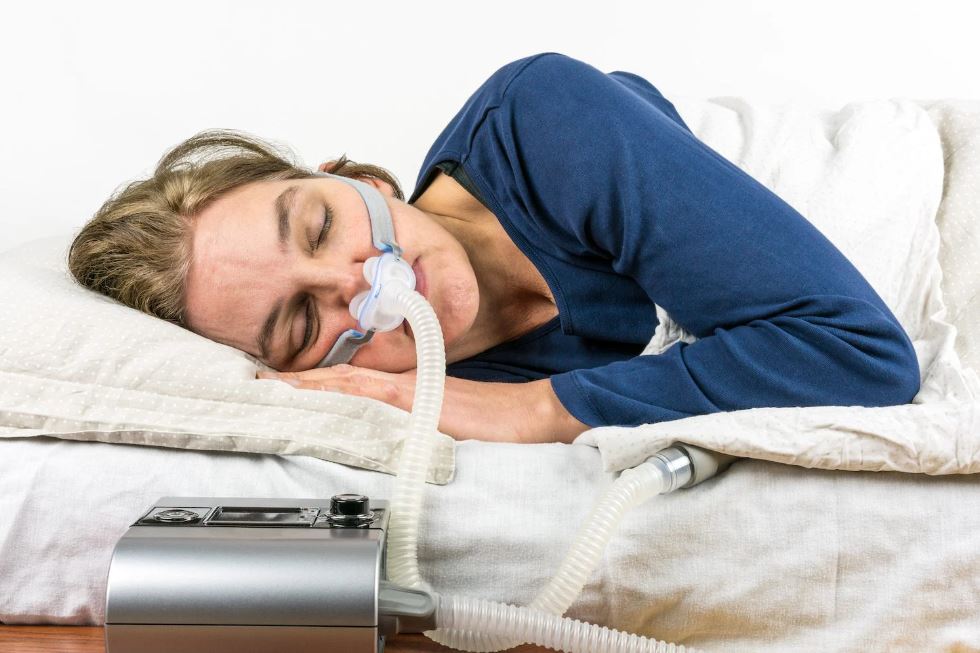
The Dysfunctional Relationship Between Obstructive Sleep Apnea and Hypertension
Independent of other risk variables like weight, several studies suggest that people with OSA are more likely to develop hypertension. It appears that sleep apnea is linked to diastolic or combination systolic/diastolic hypertension more so than systolic HTN alone. One’s risk of developing hypertension is increased by 50% in those with moderate sleep apnea, defined as an apnea-hypopnea index (AHI) of 5-15 (an average of 5-15 irregular breathing occurrences per hour). An AHI between 15 and 30 indicates moderate sleep apnea, and those with this condition have three times the risk of developing hypertension as those without the condition. This pattern is consistent with what doctors refer to as a “dose-response curve” between OSA and hypertension: the more severe the sleep apnea, the higher the risk of hypertension. An association of this nature provides the strongest proof possible that two seemingly unrelated medical disorders are, in fact, connected.
Explaining the Link Between Sleep Apnea and Hypertension
Each episode of irregular breathing puts a significant strain on your body. Your body’s “sympathetic nervous system” will activate in response to this. The “fight or flight” response triggers a cascade of harmful physiological reactions within the body, such as a rise in heart rate and a decrease in blood oxygen levels. Systolic blood pressure has been seen to rise far into the 190s during atypical obstructive breathing episodes in studies where blood pressure was recorded directly through a catheter inserted in an arm artery.
It is hypothesised that the pathophysiology (bad physiological changes in the body) of chronic stress on the body while it should be recovering during sleep is responsible for the association between sleep apnea and hypertension.
Untreated OSA is associated with an increase in “diurnal” (daytime) blood pressure, which can progress to hypertension if left untreated. Higher morning blood pressure measurements are generally the first indicator of this problem.
Resistant Hypertension and Sleep Apnea
High blood pressure that is not well controlled by three different blood pressure drugs is considered resistant hypertension. One of the most prevalent symptoms of resistant hypertension is sleep apnea. Eighty-five percent of those with resistant hypertension are also diagnosed with obstructive sleep apnea, according to studies. A sleep apnea testing is recommended for those who have been diagnosed with resistant hypertension.

Indirect (or Secondary) Hypertension
High blood pressure condition that is caused by another health issue is called “secondary hypertension.” One of the most prevalent reasons why people develop secondary hypertension is sleep apnea. All of them are included below.
Conditions include sleep apnea, renal artery stenosis, pheochromocytoma, primary aldosteronism, chronic kidney disease, Cushing’s syndrome, and aortic coarctation are all linked to sleep deprivation.
Young, otherwise healthy people who have been diagnosed with high blood pressure should get a sleep study to rule out obstructive sleep apnea as the major cause of their hypertension.
Can Blood Pressure Be Reduced With CPAP Alternatives?
When it comes to lowering blood pressure, CPAP is the therapy of choice for sleep apnea. When CPAP was compared to oxygen therapy for treating sleep apnea, it was found to significantly improve blood pressure. This makes it logical, as we attribute the blood pressure/sleep apnea connection to the “fight or flight” reaction activating repeatedly throughout sleep, rather than the oxygen dips that are also induced by sleep apnea. Because of CPAP, the throat doesn’t have to close, thus there’s no need to go into “fight or flight” mode. Even while there isn’t a tonne of data on the effectiveness of non-CPAP sleep apnea solutions, such as oral appliances, the findings of the studies that have been conducted show that they may be just as effective.
The Impact of Sleep Apnea Therapy on Blood Pressure
The continuous positive airway pressure (CPAP) machine, or its close relative the BiPAP machine, is the gold standard therapy for sleep apnea. Using CPAP consistently has been linked to a modest but noticeable drop of roughly 3 mm Hg in blood pressure. Reducing blood pressure by just 3 mm Hg may not seem like much, but it has been shown to significantly lower the risk of future cardiovascular events including heart attack, stroke, and heart failure. In addition, it is generally agreed that those with resistant hypertension and sleep apnea will have a hard time maintaining normal blood pressure until their sleep apnea is treated. It would be fantastic if high blood pressure could be lowered without the need of drugs, which come with their own set of downsides. It is possible that a CPAP machine is the sole treatment necessary to return blood pressure to normal in those with secondary hypertension caused by sleep apnea.
Take Away
- Sleep apnea is strongly linked to hypertension.
- Sleep apnea may be the primary cause or a key contributing factor to hypertension in some people.
- Over time, sleep apnea causes daytime hypertension by preventing the natural lowering of blood pressure that occurs during sleep.
- Sleep apnea testing is recommended if your high blood pressure is resistant to treatment.
- In the long run, untreated sleep apnea can lead to hypertension.
- Those with hypertension should be given a CPAP or BiPAP equipment to help with their sleep apnea.
- Lowering blood pressure and improving heart health, as shown in the prevention of cardiovascular diseases including heart attack, stroke, and heart failure, are two of the many benefits of treating sleep apnea with a CPAP machine.

